New Pre-Scleroderma Classification May Help Manage Disease, Predict Outcomes
Written by |
A recent study showed that the classification of patients with pre-scleroderma into “very early systemic sclerosis” (SSc or scleroderma) and “early SSc” groups — based on the existence of subclinical organ involvement — can help improve disease monitoring and care, and better predict patients’ outcomes.
The study also showed that patients in the early SSc group progressed to full-blown systemic scleroderma more often than those in the very early SSc group. Pre-scleroderma patients whose digestive system was affected by the illness were also found to be at greater risk for developing SSc.
The study reporting the findings, “Very early and early systemic sclerosis in the Spanish scleroderma Registry (RESCLE) cohort,” was published in the journal Autoimmunity Reviews.
The study examined the records of 1,632 patients with SSc from the Spanish Scleroderma Registry (RESCLE). Of them, 36 (2.2%) were re-classified within the very early SSc group, and 111 (6.8%) within the early SSc group.
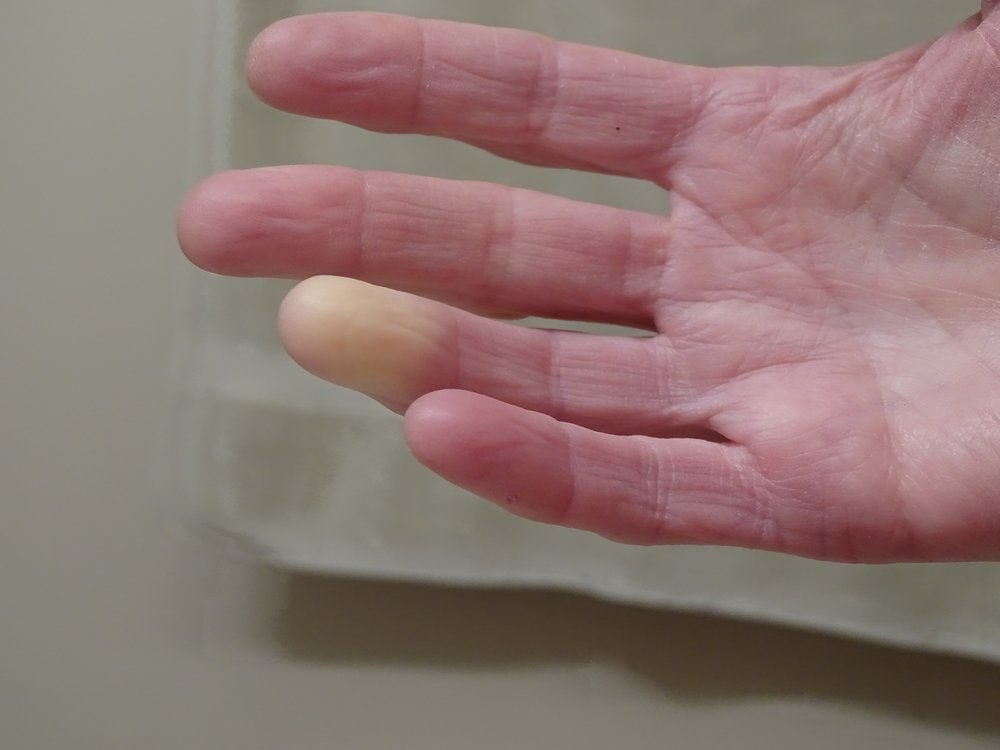
All patients classified in the very early SSc and early SSc groups had Raynaud’s phenomenon, a condition that involves spasms in blood vessels causing color changes in fingers and toes (going from pale to blue to red), usually after exposure to cold temperatures.
The two groups were similar to each other in the proportion of males and females, in age at which the illness began, and how long Raynaud’s phenomenon lasted.
They were also similar as to whether they had antinuclear antibodies (antibodies that can cause organ and tissue damage and are typical of autoimmune diseases), and in capillaroscopic findings — capillaroscopy looks at abnormalities in tiny blood vessels and is used to diagnose SSc.
In total, three very early SSc patients (8.3%) evolved to definite SSc, while 31 patients with early SSc (28%) evolved to a definitive SSc diagnosis.
“The importance of an early diagnosis lies in the possibility to anticipate complications with close monitoring. The period between identifying patients with initial manifestations to the development of irreversible organ damage constitutes a ‘window of opportunity’,” the team wrote.
Researchers also found that patients whose disease involved the digestive tract were more likely to progress to a definitive SSc diagnosis.
“The evolution to definite SSc is more frequent in early than in very early SSc patients. Digestive involvement is a risk factor of progression. An active assessment of organ damage in preclinical stages allows a correct classification and risk stratification, with implications for monitoring and treatment,” the researchers concluded.





