50 Shades of Blue

Here in the U.K., autumn has arrived. The color changes of the natural landscape at this time of the year are stunningly beautiful. This annual display of nature showing off its true colors provides a reminder that winter is on its way. And winter is the nemesis season for me and every patient with a similar diagnosis.
Sadly, my daily reality is that the severity of my Raynaud’s involvement keeps me under house arrest year-round.
I must wear thick, fleecy socks, UGG boots, and gloves in an attempt to prevent a Raynaud’s attack, as there is no cure.
My sensitivity is such that the smallest decrease in temperature, regardless of how warm, will trigger a Raynaud’s attack in my hands and toes. My ears and nose may also become involved.
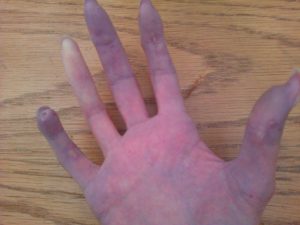
My hands and feet are very rarely the same pinkish color as a “normal” person. My “normal” is a paler pink.
For me, color changes occur in every Raynaud’s attack.
At the onset of a Raynaud’s attack, my pale pink will turn to white, visibly showing that there is total blood loss to that particular body part.
Depending on the severity of the Raynaud’s attack, the white discoloration may be preceded by a blue tinge to the body area. During the white color stage, it is impossible for me to feel anything in the body area that is affected.
For example, my hands or feet — whichever area is affected on a particular attack — will feel numb and extremely cold. My toes and fingers will become extremely rigid. This is painful and extremely debilitating.
When the body area warms, the color changes begin. This means blood is gradually returning to the affected area.
The rigid white will gradually transform into a very dark blue, which will then slowly change into lighter shades of blue as the body area warms.
While the blood returns to the vessels, the pain is excruciating. There are no words that come close to describing this horrific sensation.
Maybe “slamming your hand in a car door,” or, “having that body part torched with hot pokers.”
Total exhaustion follows.
A few years ago, I was horrified to see my hands turn black due to being out in the cold for too long. This happened even while wearing my compulsory “polar Bond Girl uniform.”
Prevention of an attack is crucial since there is no cure.
During the course of my global patient profiles campaign for Scleroderma Awareness Month in 2017 and 2018, every patient detailed how Raynaud’s and digital ulcers were a continuous problem.
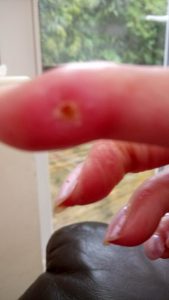
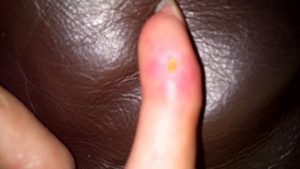
The digital ulcer that appeared in March on my right index finger still remains in situ. This appeared to be from excessive keyboard use in March, which was Autoimmune Disease Awareness Month. Hence my absence from social media for the last month.
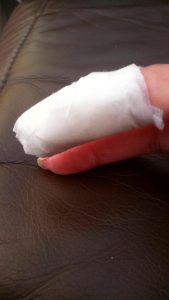
A thick, self-made, padded bandage with minimal adhesive helps to protect the very tender, thin, red, raw skin.
However, I know that when it comes to digital ulcers, I am very lucky, even though the pain and daily management is extremely soul-testing.
Combined with calcinosis, this makes for a very painful and debilitating reality.
Other unmet clinical needs that patients have in common include:
- Calcinosis;
- Gum recession and tooth extracts;
- Soft tissue and ulcers;
- Telangiectasia;
- Sclerodactyl hands;
- Invisible disability;
- Raynaud’s;
- Gastrointestinal;
Although these unmet needs are not immediately life-threatening, they cause havoc with the day-to-day quality of each patient’s life.
An investment in medical research will most certainly improve the current soul-destroying reality that these unmet clinical needs bring.
I am honored to be a patient research ambassador with the National Institute for Health Research. Watch a video about this.
Overall, for optimum patient care, three hallmarks preside:
In the meantime, I continue to remind myself that “My Job Today is to Simply Get Better,” with hope and my canine diva dream team as my constant companions.
Living the dream, scleroderma style.
Follow:
Facebook Page: Raynauds Scleroderma Awareness Global Patients
Twitter: @SclerodermaRF @RaynaudsRf
Google Plus: RaynaudsSclerodermaAwarenessGlobalPatients
#SclerodermaFreeWorld #RaynaudsFreeWorld
#IamScience
Please DONATE to help fund medical research at The Scleroderma Unit, The Royal Free Hospital, London.
When donating, 100 percent of your monies will be used for medical research purposes only. Thank You.
October is Raynaud’s Awareness Month
***
Note: Scleroderma News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Scleroderma News or its parent company, Bionews Services, and are intended to spark discussion about issues pertaining to scleroderma.

















Leave a comment
Fill in the required fields to post. Your email address will not be published.