Increased Skin Pigmentation Lesions May Help Predict Course of Systemic Sclerosis, Study Suggests
Written by |
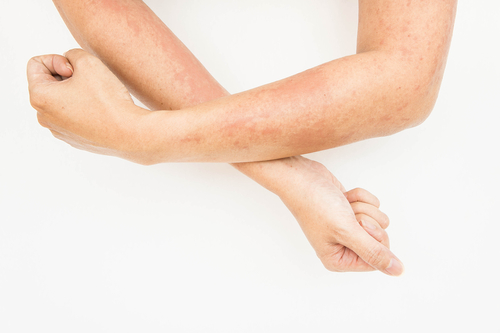
Evaluating changes in skin pigmentation could be useful for the management of systemic sclerosis (SSc) patients, particularly to identify those at risk of developing digital ulcers, researchers suggest.
This finding was reported in the study, “Association of skin hyperpigmentation disorders with digital ulcers in systemic sclerosis: analysis of a cohort of 239 patients,” published in the Journal of the American Academy of Dermatology.
In recent years, several advances have been made to improve the diagnosis and management of SSc. However, its course of progression remains unpredictable, with severe organ damage and vascular complications representing a challenge for clinicians and patients.
Between 30.5% and 91% of patients have skin pigmentation disorders related to SSc. These more frequently affect patients of Hispanic and African-American descent rather than Caucasians, suggesting that such skin manifestations may be associated with darker skin types.
To date, despite several reports describing different types of skin pigmentation disorders in SSc patients, their prevalence and association with the disease has not been fully characterized.
The study, aiming to address this, enrolled 239 patients with confirmed SSc, of whom 70.7% had limited cutaneous SSc and 29.3% diffuse cutaneous SSc.
A total of 88 patients were found to have skin pigmentation disorders: 58 had increased pigmentation (hyperpigmentation); 35 had reduced pigmentation or hypopigmentation. Five patients had both types of alterations.
About 68.2% of these patients had a lighter skin tone (phototype II to III), while 30.7% had darker skin (phototype IV to V).
Taking into account patterns of skin pigmentation, researchers found that 34 patients had diffuse hyperpigmentation; 24 had hyperpigmentation limited to sun-exposed areas; nine presented hypopigmented flecked macules localized on the forehead, neck and upper chest and back; 11 patients had hypopigmented lesions spread over the body; and 15 had hypopigmented macules limited to the peripheral areas.
Collectively, the data revealed that hyperpigmentated lesions were more frequent among patients with diffuse SSc, in particular diffuse hyperpigmentation. Hyperpigmentation was also found to be associated with higher Rodnan skin scores (mRSS), which is a measure of skin thickness.
Further analysis showed that the onset of Raynaud’s phenomenon — a complication of SSc resulting from the constriction of blood vessels in the extremities — less than 10 years after the appearance of SSc was significantly associated with hyperpigmentation.
In addition, SSc patients with diffuse hyperpigmentation were found to have a 2.96 times higher risk of having vascular problems and consequent complications, such as digital ulcers. Researchers found a positive association between diffuse hyperpigmentation and the presence of digital ulcers.
“We clearly demonstrate that diffuse hyperpigmentation is related to digital ulcers, a symptom of vascular involvement in SSc,” the researchers wrote. “[This is] of great interest because we have recently demonstrated that digital ulcers could be associated with increased risk of mortality in patients with SSc.”
Based on these findings, the team believes that “screening for hyperpigmentation disorders could be useful in the management of SSc patients. It could help in the diagnosis of patients “when faced with early undifferentiated symptoms,” but also “as a marker to identify patients who are most at risk of developing digital ulcers and/or vascular involvement,” they said.





